Offer more than just technology
Do you want to revitalize effective communication for your patients, especially those with severe and profound hearing loss? Dr. Linda Thibodeau suggests that we put a stronger emphasis on non-technology strategies. This means focusing on solutions that involve the human connection.
As hearing care professionals (HCPs) we strive to determine the unique challenges a person with hearing loss may experience and then offer an array of solutions. With all the advances in technology is it easy to think of the digital features on ear level devices that may address an individual’s personal communication challenges. Of course there are important non-human communication needs such as hearing smoke alarms, telephones, and doorbells or an announcement from Alexa.
Advances in wireless connectively have resulted in an increased need for the HCP to guide the consumer in developing a wireless technology plan in order to efficiently solve communication demands with the fewest number of devices.1 Perhaps overall success can be enhanced by focusing on REVITALIZING effective communication interactions with persons they encounter on a daily basis.
Irony of meeting communication needs with technology
It seems ironical that in our efforts to restore communication with humans, we often place a stronger emphasis on a solution that is non-human and may overlook many solutions that involve changes in human interaction.
We have all heard many examples of non-productive communication practices that often preclude one from the benefits of expensive features on personal technology. For example, with Art who wears hearing aids and his wife Arlene, even the highest-level technology may not allow accurate understanding if she is simultaneously making a phone call while giving instructions to Art who has a newspaper in front of his face.
He is not even trying to focus on her voice because he rightfully assumes she is making a phone call that does not involve him. If such practices are not addressed as part of a foundation of communication, persons may become frustrated with the expensive technology and ultimately return it.
Traditional aural rehabilitation programs
The late Mark Ross provided HCPs a wealth of information about these human factors to improve communication as he experienced hearing loss following WWII and subsequently developed effective programs to teach strategies, speech reading, and auditory training to supplement the basic technology available at the time.2
However, advances in technology led to programmable aids and real ear verification, both of which provided colorful displays. It seems that as these displays became the basis for explanations of how digital technology could overcome audibility deficits, the ’less colorful’ aural rehabilitation topics were not addressed.
To make such a program easily accessible for the HCP, Louise Hickson and colleagues developed and validated a protocol for Aural Rehabilitation, known as Active Communication Education (ACE), that includes six modules to address common communication challenges such as communicating in background noise, in the home, and with difficult speakers.
The program is designed to be conducted in a group setting for two hours per week over five weeks. Although the value of this programs has been well established,3 lack of reimbursement often remains a major obstacle to implementation.
Importance of graduate education
One solution to the focus on technology with less attention to non-technology strategies could start with the curriculum in Doctorate of Audiology programs. If future HCPs receive limited exposure to the benefits of the programs, they are likely not to initiate programs in their own clinical practice.
This was the impetus for an Advanced Aural Rehabilitation course at the University of Texas at Dallas (UTD) Callier Center, called SIARC, or Summer Intensive Auditory Revitalization Conference.5
Description of SIARC:
• This is a five-day workshop (2 half days and 3 full days) where couples are paired with AUD graduate students to complete four classes daily that are very similar to Ross and Hickson’s programs. Starting with a complete needs assessment, the goals are developed for the individual that includes technology (use of personal and remote microphone systems) and non-technology solutions (communication strategies, coping skills, speechreading/auditory training).
• The program includes events to ‘practice’ with the technology and non-technology solutions in the real world through dinners in noisy restaurants and tours of public facilities such as museums, the arboretum or theatre productions. By engaging in these group activities over the five days, bonds are developed among the participants that help to build a firm foundation for success.
• Students can reinforce the use of all the solutions in the real-world situations which helps them witness the benefits and understand the value of incorporating both the technology and non-technology components in service delivery. The participants are grateful for the opportunity and strategies with the immediate assistance provided by the students. The technology generously provided by Phonak is available for use in other training programs to start such a program. A guide for the development of SIARC is available at SIARC – Hearing Health Lab – The University of Texas at Dallas (utdallas.edu)
From SIARC to clinical practice
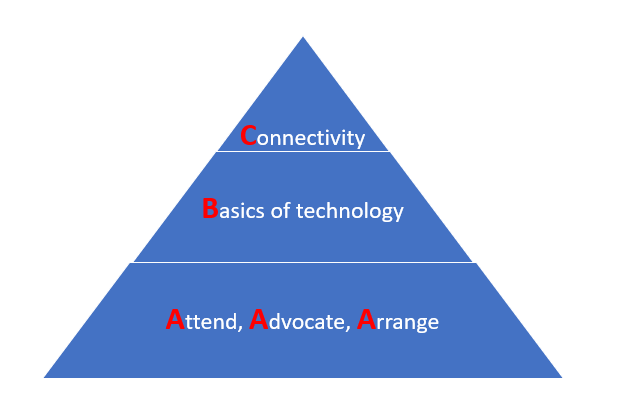
Even after an intensive training experience, HCPs may find it difficult to focus on the non-technology solutions in a busy clinical setting. Let us revise the comprehensive nature of the ACE program or SIARC into a simple three-layer pyramid that could prompt HCPs to address these topics routinely with their patients.
Just as the TELEGRAM was developed as a system to prompt HCPs to conduct a needs assessment in several areas (Telephone, Employment, Legislation, Entertainment, Groups, Recreation, Alarms, Members of the family),6 the Pyramid of Communication Success can prompt the HCP to develop a foundation of non-technology skills upon which to introduce technology. The combination of skills and technology can lead to successful communication.
Layer 1 – Human factors :
Attend and get attention – First step is talker to get the listener’s attention and then they can attend to the message.
Advocate with feedback – Once communication has started, the listener must advocate for their needs and let the talker know if they need a slower rate or rephrasing, etc. Simply asking the talker to use ‘clear speech’ can result in a significant improvement in speech recognition.7 The talker will likely increase the desired behavior if he/she receives feedback such as “Thank you for slowing down, that is exactly what I needed.”
Arrange the environment – Both the talker and the listener can survey the environment and determine ways to improve the situation such as reducing background music, increase the lighting, or move to another location.
Layer 2- Non-human factors:
Basics of technology – Once the foundation of non-human solutions is established, the basic features of technology may be introduced starting with restoring audibility. Based on the needs assessment more sophisticated features could be considered that address personal challenges. For example, a golfer might want to try a wind reduction program or an executive might want sophisticated noise reduction and directional microphone options as well as compatibility with remote microphone systems
Layer 3- Blending Human and Non-human factors:
Connectivity – The peak of the Pyramid of Communication Success involves the connectivity features of the personal technology with remote microphone technology or smartphones to achieve maximum success. The foundation components are also critical to the successful use of the technology. The listener must advocate for the use of the remote microphone by the talker which will facilitate attending to the message. The listener can then provide feedback regarding the benefits achieved in the acoustic environment that has been optimized for communication. The stronger the foundation, the higher the pyramid can be built, or in this case, the greater the success.
Conclusion
It is well established that group Communication Enhancement sessions are beneficial to the individual with hearing loss and their families. The importance of human and non-human (technology) solutions must be included in the graduate education programs.
When a comprehensive multi-day group program cannot be offered, review the ABCs in the Pyramid of Communication Success with every patient: Attend, Advocate, and Arrange followed by Basics of technology, and then Connectivity between the human and non-human components.
To learn more on the clinical management for those with severe and profound hearing loss, we recommend you read the full text of the recent publication available through Open Access in Seminars in Hearing, Guidelines for Best Practice in the Audiological Management of Adults with Severe and Profound Hearing Loss.
To learn more about the ACE protocol, please read Professor Louise Hickson’s blog article on the program she developed in collaboration with colleagues at the University of Queensland.
 Dr. Linda Thibodeau to be featured in podcast series
Dr. Linda Thibodeau to be featured in podcast series
The podcast, ‘The Audiologist’ launched a new series based on content in the severe and profound guidelines. It delivers informative interviews with the experts who created them.
Dr. Thibodeau will be one of the experts interviewed in coming weeks and will further discuss non-technology solutions to improve communication for those with severe and profound hearing loss.
Find the series here.
References
1. Thibodeau, L & Panahi, I. (2021) Smartphone Technology: The Hub of a Basic Wireless Accessibility Plan. The Hearing Journal, 74, 6-7.
2. Hearing Review (2021). Tribute: Mark Ross, PhD, a Founding “Father of Aural Rehabilitation”. https://www.hearingreview.com/inside-hearing/people/tribute-mark-ross-father-of-aural-rehabilitation, accessed July 14, 2021.
3..Hickson,L., Worrall, L., & Scarinci,N. (2021). ACE: Active Communication Education A program for adults with hearing loss. Retrieved from https://shrs.uq.edu.au/files/122/ACE%20Booklet%202.pdf, accessed July 14, 2021.
4. Hickson,L., Worrall, L., & Scarinci,N. (2007). A Randomized Controlled Trial Evaluating the Active Communication Education Program for Older People with Hearing Impairment. Ear and Hearing, 28, 212-230.
5. Thibodeau, L. & Cokely, C. (2003). Maximizing Auditory Rehabilitation Training for Clients, Students, and Faculty through SIARC: Summer Intensive Aural Rehabilitation Conference. Journal of the Academy of Rehabilitative Audiology, 36, 67-82.
6. Thibodeau, L. (2008) Page Ten: How the TELEGRAM can help your patients “Reach out and touch someone!” Hearing Journal, 61, 10-17.
7. Krause , J. & Panagiotopoulos, A. (2019) Speaking Clearly for Older Adults With Normal Hearing: The Role of Speaking Rate. Journal of Speech, Language, and Hearing Research, 62, 3851-3859.